
The client needs to be at the end of the hall because he requires privacy b. A minimum of 12 air-flow changes each hour must be maintained in order to sustain the desired environment and depending on. The preferred method for cough-inducing procedures is the use of a local exhaust ventilation device such as a booth or special enclosure. However actual experiments have proven that increasing airflow rates. We always follow and recommend AIA guidelines. Negative room pressure is an isolation technique used in hospitals and medical centres to prevent cross-contaminations from room to room. The room is also sealed to avoid external air leaks and avoid additional. Negative pressure causes air to flow from the corridors into the AII room.Ĥ It is unnecessary for a patient to wear a P2N95 mask. 
AII rooms have negative pressure relative to other parts of the facility. A negative pressure room is an optional requirement for sputum induction procedures.Ĭhickenpox tuberculosis severe acute respiratory syndrome SARS-CoV Middle East respiratory syndrome MERS-CoV and coronavirus disease 2019 COVID-19. Negative Pressure Isolation Rooms Tuberculosis TB Isolation Rooms AirMont Inc. Respiratory and contact isolation of symptomatic patients and their contacts in negative. The ANSIASHRAEASHE Standard 170-2008 makes recommendations for hospital critical care spaces in regards to negative and positive. AII rooms have the following characteristics. They explicitly call out OA and Room Air Changes ACH for Infectious Disease negative or Immuno-Defficient positive Rooms and also positive or negative adjacent relationships. This study was based in Lima Perus capital city. The need for such controlled spaces has increased dramatically in light of the COVID-19 pandemic. Negative room pressure is an isolation technique used in hospitals and medical centers to prevent cross-contamination from room to room. Tuberculosis Infographic Medical Photos Medical Awareness Respiratory Therapy If these rooms are not being used for patients who have suspected or. Airborne infection isolation AII rooms are negative pressure rooms designed to prevent airborne pathogens released from patients with illnesses like tuberculosis from recirculating in the air 1 read more on how TB spreads from the CDC here. There is a strong argument for advising ventilated facilities and personal respiratory protection for the care of all patients with tuberculosis, as multi-drug tuberculosis may not always be apparent on admission, and these measures minimise transmission of all cases of TB to other patients and healthcare staff.This Rapid Response review aimed to identify available evidence on the clinical effectiveness of portable or temporary negative pressure rooms and related evidence-based guidelines for the management of people with active tuberculosis. The differences in recommendations may reflect the variations in epidemiology and the greater use of BCG vaccination in the UK compared with the United States. Even when policies and facilities are optimal, there is a need to regularly review and audit these as sometimes compliance is less than optimal. Nonetheless, observational studies and mathematical modelling suggest that all measures are required for effective prevention. The absence of clinical trials in this area precludes dogmatic recommendations. In the US, the standard of care for patients with infectious tuberculosis is a negative pressure ventilated room and the use of personal respiratory protection for all healthcare workers entering the room of a patient with suspected or confirmed tuberculosis. filtered masks, are not considered necessary unless multi-drug resistant TB is suspected, or where aerosol-generating procedures are likely. In the UK, however, negative pressure isolation rooms are recommended only for patients with suspected multi-drug resistant TB and personal respiratory protection, i.e. 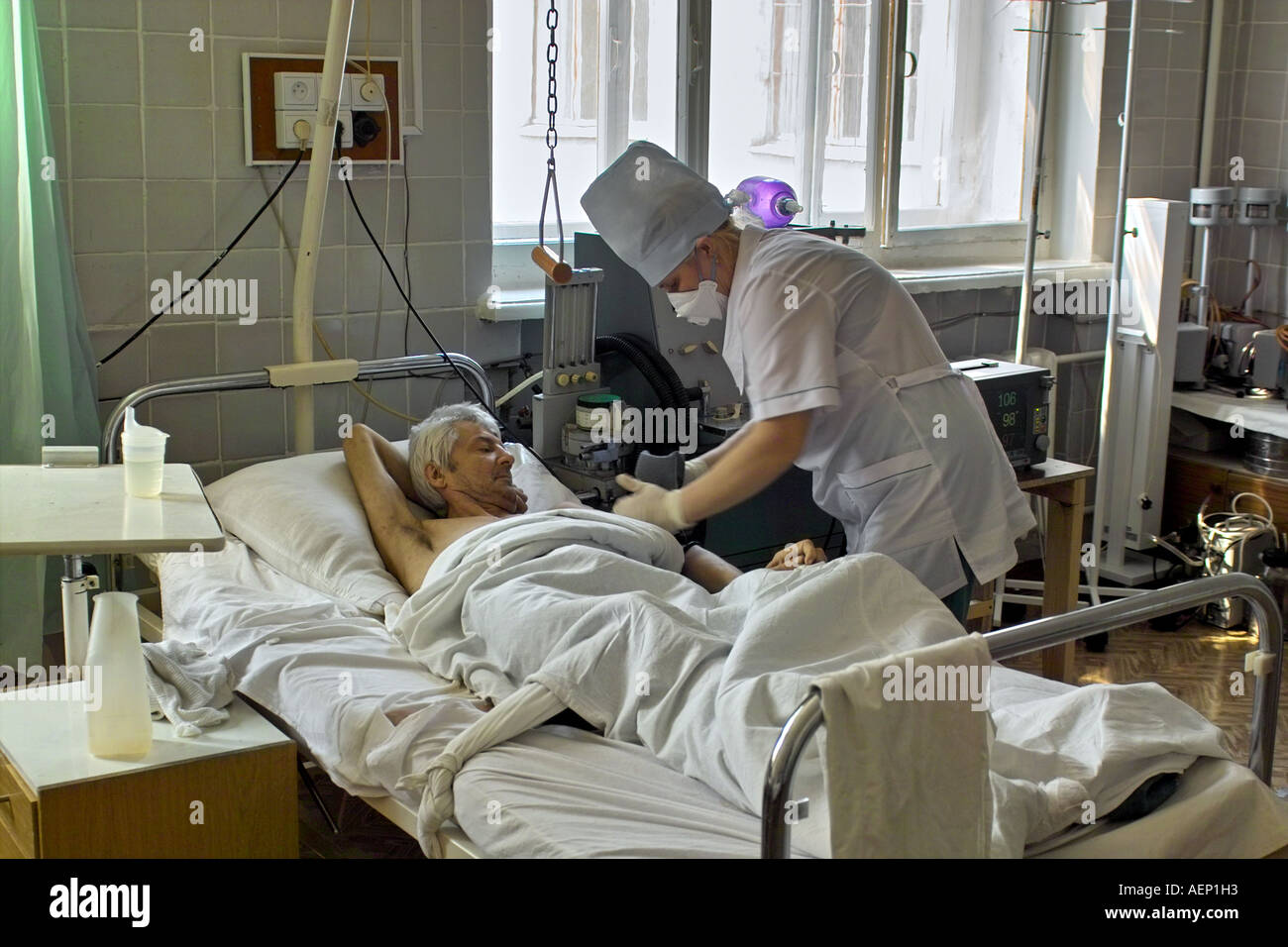
Recent guidelines on the prevention of tuberculosis in healthcare facilities from Europe and the USA have many common themes. 
ventilated isolation rooms) and personal respiratory protection (face sealing masks which are filtered). The control and prevention of tuberculosis in hospitals is best achieved by three approaches, namely administrative (early investigation diagnosis, etc.), engineering (physical facilities e.g. Outbreaks of healthcare-associated tuberculosis are usually associated with delays in diagnosis and treatment, or the care of patients in sub-optimal facilities. Although the prevalence of tuberculosis continues to decline in most developed countries, the risk of healthcare-associated tuberculosis, remains for patients or healthcare staff.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
